May 1, 2004
Mr. I.T.P. was a young upwardly mobile stockbroker who had just moved into a new home near the commuter line with his wife and two small boys.Ā He recently had noted that when he brushed his teeth, they would bleed easily, and his wife commented that when he came home from work, his legs and arms were bruised which he attributed to bumping his desk.Ā One night, while rough-housing with his sons, he accidentally struck his head against the door jamb as he was chasing them into bed.Ā He fell back on the ground striking the back of his head and for a moment felt a bit dizzy.Ā But he recovered quickly and tucked his sons into bed and kissed them good-night.Ā He told his wife that he needed to get to bed early because of a conference call that he needed make at the office early the following morning.Ā Unaware of her husband’s potential problem, his wife blew him a kiss as she continued to read her book.Ā On coming to bed she found Mr. I.T.P. to be unresponsive.Ā She called “911” and EMS arrived and whisked him to the hospital.Ā But he was D.O.A.
Mr. D.I.C. was a 55 year old cab driver who presented to the hospital with severe crushing central chest pain.Ā His doctors suspected that he had severe coronary artery disease and after being stabilized in the emergency room, he was taken to the cardiac cath lab and then to the operating room where an emergency coronary artery bypass procedure was performed.Ā His family and friends crowded into the surgical waiting room hoping to be able to hear that all had gone well.Ā The surgeon approached his wife and told her that although Mr. D.I.C. had made it through the operation, he had dropped his blood pressure several times during it, but he seemed to be holding his own for now.Ā He cautioned her that sometimes with these sorts of things happen, other organs can shut down and that her husband would be closely monitored in the coronary care unit.Ā Just as the surgeon had predicted, Mr. D.I.C. was noted to develop problems with kidney and lung function, thought to be due to the episodes of shock that he had experienced during the operation. Suddenly, he was noted to develop severe bleeding from several I.V. sites and he started to vomit and defecate large amounts of blood almost simultaneously.Ā Within several minutes, despite being given massive amounts of Āfluids, blood products and medications, Mr. D.I.C. went into irreversible cardiac arrest and died.
Mrs. A.P.C-R. was a young law student who started to notice some vague calf pains associated with increasing swelling of her legs just a few days before her final exams. Unperturbed, she continued her usual activities although her leg pains seemed to worsen when she was up walking around. ĀShe decided to forgo her usual pre-test workout at the gym which usually relaxed her because she just didn’t feel herself.Ā On her way to the exam she started noticing that she was a bit short of breath if she tried to walk fast.Ā So she slowed down and tried to pace herself.Ā She thought that maybe she was just out of shape, coming down with something, or was just nervous.Ā Once inside the examination hall she started to relax and feel like herself again.Ā But about one hour into the exam, she started to notice some vague rib ache and became very short of breath.Ā An examination monitor noticed her fidgeting around and came over to see what was the matter.Ā She reassured him that she sometimes would get nervous in these situations and given some air she’d probably recover in time to finish the exam.Ā As the monitor turned to check to see what the professor would want done in this situation, he heard a loud thud.Ā Mrs. A.P.C-R had collapsed on the floor behind him and she was no longer breathing.Ā The monitor signaled for someone to call “911” and immediately began CPR on the young law student, but it was to no avail.
What do all of these people have in common, other than being dead?Ā What do you suppose has ultimately been responsible for their sudden deaths? ĀHemostasis; the process by which the body is physiologically able to stop bleeding, is the culprit here.Ā Maybe too little or maybe too much.Ā You have to have just the right amount in the right situation in order to sustain life.Ā If it turns off, or it turns on, at the wrong moment, you may end up like these three patients; suddenly dead.
Read on to learn more about the intricacies of how the body balances its need to prevent blood loss from bleeding while at the same time allowing for the free flow of blood in the circulation.Ā Along the way, keep in mind that those who promote the validity of macroevolution, expect us to believe that this interdependent, extremely complex system for controlling bleeding in the body, developed one step at a time while still allowing a multi-system organism with a complex body plan to survive each step along the way.Ā
As we go through how the body accomplishes hemostasis, we’ll not only learn what happened in each of these cases, we’ll also show you how other similar defects resulting in hemostatic dysfunction can result in the same outcome; death.Ā As I’ve said before; there are many pathways to death.Ā The more complex a machine is, the more ways that it can malfunction.Ā The proposed “one step at a time” mechanics of macroevolution seems to defy this universally recognized premise.Ā Only by understanding that the cell, and consequently the body as a whole, must maintain a very narrow range of various chemicals within itself in order to survive, does one come to realize that macroevolution, as it is currently being taught, is not sufficient to explain what all rightly understood biological function presents as evidence against it.
Overview of Hemostasis
When we talk about how the body is able to control any bleeding that may
occur within it, we need to consider four different mechanisms that are always
working simultaneously.Ā The first is the compensatory reaction of the blood
vessel that is injured.Ā The second is the action of platelets in the bloodstream.Ā
The third is the effect of clotting factor proteins in the circulation.Ā The
fourth is the anti-clotting mechanisms that are present within the body that
act as a counterbalance to coagulation.Ā We only want clotting to occur when
there’s a danger of bleeding.Ā Otherwise we could clot off our entire circulation
and then where would we be?Ā In one word: dead!!
In summary, there is a constant “give and take” going on in the body regarding the formation and prevention of clots.Ā Once the system is turned “on” there has to be a mechanism to turn it “off”.Ā I hope to impress upon you the fact that within each of these above-mentioned four components of hemostasis, lies an irreducibly complex system of molecular reactions.Ā But equally important is the fact that the function of hemostasis, comprised of these four separate mechanisms, is itself irreducibly complex as the cases of Mr. I.T.P, Mr. D.I.C. and Mrs. A.P.C-R. will clearly demonstrate.Ā Be prepared to exercise your wonder as you never have before.Ā For when you’ve finished this column you’ll be totally amazed!!ĀĀ
Vascular Function
When a blood vessel is injured certain chemicals are released from platelets
and other cells nearby which make the smooth muscle that surrounds the blood
vessel contract.Ā This results in an action called vasoconstriction which causes
the opening in the blood vessel to diminish, sometimes down to nothing.Ā This
plays a significant role in helping the body to stop bleeding.Ā As the blood
vessel tries to close off as much as it can, the second mechanism for hemostasis
kicks in: the platelets.Ā Think of what happens whenĀ someone is trying to close
a fully packed suitcase by pushing both ends together while someone else applies
the lock.Ā The platelets and the clotting factors together apply the lock as
best they can, but without vasoconstriction their task would be almost hopeless.
In general, if the whole system for hemostasis is working properly, only deep cuts that may involve the disruption of a major vein or artery, or penetrating and high impact trauma that may cause serious injury to a major organ such as the spleen, the liver or the kidney, tend to cause enough bleeding to be life-threatening.Ā Sometimes an injury or spontaneous bleeding can occur in a vital area of the body, such as the brain.Ā Bleeding here can be life-threatening because the brain is encased in the skull and if bleeding is excessive, the pressure of the blood pressing on the brain will cause injury to the nervous tissue.Ā If too much pressure builds up, the areas of the brain that are responsible for awareness, wakefulness, respiration and the heart beat, may be destroyed and death will ensue in short order.Ā And many times, people will have spontaneous bleeding from the gastrointestinal system due to various disorders.Ā If left unchecked, this may cause the person to lose so much blood that the body is not able to maintain its vital functions and death will occur.Ā Therefore, having an underlying vascular abnormality can sorely test the hemostatic system of the body since the blood vessel itself is defective.ĀĀ
There are several rare conditions in which the body contains abnormal vessels which have difficulty contracting on injury.Ā One example of this is the Osler-Weber-Rendu Syndrome in which the patient has a tendency to bleed due to abnormal blood vessels which are prone to spontaneous bleeding in critical areas of the body.Ā Another problem can be excessive vascular fragility which is often associated with many chronic illnesses, and which puts people at higher risk for spontaneous bleeding or significant bleeding with minimal trauma.Ā Life-threatening hemorrhage can occur if a major organ or vessel is involved.Ā
Clearly, normal vascular function is necessary for adequate hemostasis in the body. The complicated structures surrounding all blood vessels allow for the proper flow of blood while at the same time being able to minimize bleeding when injury occurs.Ā Each component of the blood vessel wall is important to allow for efficient blood flow.
Platelets
Platelets are formed from cells called megakaryocytes, that originate
from the bone marrow.Ā These cells break off bits of themselves to become platelets.Ā
The formation of megakaryocytes, and therefore platelets as well, is regulated
by a chemical messenger called thrombopoietin which appears to
be derived from the liver, the kidney, the spleen and the bone marrow itself.Ā
The thrombopoietin is able to attach itself to receptors on the primitive stem
cells in the bone marrow to stimulate them to mature into platelet prod-ucing
megakaryocytes.
The platelet is basically a piece of cellular cytoplasm that is surrounded by a cell membrane that contains organelles which allow it to function and little granules that contain numerous active proteins.Ā But the platelet does not have a nucleus.Ā Normally, platelets circulate throughout the bloodstream without interacting with each other or other cells.Ā But if the platelet is exposed to a proper stimulus, such as an injured blood vessel, it will become activated and then it will start to stick to other cells or tissue nearby.Ā All blood vessels are lined with a tissue called endothelium which generally does not activate platelets.Ā Just below the endothelium is support tissue that contains a protein called collagen.Ā When platelets are exposed to collagen they become activated and start to stick together and this is what stimulates the platelets to continue the hemostatic process.Ā
So when you slip and fall against a sharp rock and you break some of the small blood vessels in your skin, this exposes the platelets in your bloodstream to the collagen below the surface of the damaged blood vessels.Ā Another way that collagen can be exposed to platelets in the bloodstream is when a cholesterol plaque that’s attached to the endothelium of a blood vessel, such as in the heart, breaks away and pulls some of the endothelium with it.Ā This will cause the platelets that are floating by to become activated and they will start to stick together and form a soft clot, called a thrombus.Ā This is part of the mechanism behind how clogged arteries in the heart can totally plug up and cause a heart attack.Ā Another name for a heart attack is a coronary thrombosis.
The way that platelets are able to adhere to become a thrombus involves three main factors.Ā First, the combination of collagen exposure and the release of other nearby chemicals from the injury allows platelet cell membrane receptors to be activated and this causes the platelets to stick to each other and other cells.Ā Both the plasma and the platelets also contain a protein called Von Willebrand Factor which is chemically able to allow the adhering platelets to take hold and start a thrombus within the breach that is being reduced by localized vasoconstriction as described above.
Next, the activated platelets are capable of releasing several chemicals from the granules contained in the cytoplasm, which have the combined effect of recruiting other platelets and activating them to stick to each other.Ā Think of it as a huge chemical tractor beam. ĀAspirin, in proper doses, is able to partially block the effects of some of these chemicals that promote the activation, recruitment and stickiness of platelets.Ā That’s how it seems to prevent heart attacks and strokes.Ā
But there is also a third factor that plays a major part in completing the thrombus.Ā It’s a protein that’s produced in the liver called fibrinogen.Ā The platelet has a receptor for fibrinogen on its cell membrane.Ā When thousands and thousands of fibrinogen molecules, in the presence of calcium ions, lock onto the platelets through these receptors, the thrombus begins to become stronger.Ā The thrombus that is formed is very soft and it usually is not adequate to permanently stop the bleeding.Ā Think of the thrombus as a temporary filling that the dentist puts in until you come back in the office for the permanent one.Ā That’s when the clotting factors come into play.Ā But before we go on, let’s look at what can happen in the body when there aren’t enough platelets or they aren’t functioning properly.Ā
Remember our first case-study, Mr. I.T.P.?Ā That’s what happens when everything else in the hemostatic system is working except the platelets.Ā I.T.P. stands for idiopathic thrombocytopenia, a condition in which the platelet count in the blood is often less than 10% of the acceptable lower limit.Ā There are numerous diseases that can result in either low platelet counts or poorly functioning platelets.Ā Most of these people die from serious bleeding, often from minor trauma, or spontaneously, because the platelets aren’t able to form a proper thrombus to facilitate coagulation. ĀIn Mr. I.T.P.’s case, his bleeding tendency resulted in a life-ending hemorrhage within his brain from the minor head trauma that he suffered when playing around with his boys.Ā Maybe now you can see why platelets are so important.Ā ĀĀ
A cursory review of platelets, how they function, where they come from, and how their production is controlled, shows that several factors must be in place for adequate thrombus formation to occur.Ā Clearly this intricate system is irreducibly complex in that if any one of these components were to be missing, the whole system would fail, thrombus formation would not occur, and the multi-system organism would suffer the fate of Mr. I.T.P.Ā Below are only the components responsible for platelet function that I’ve mentioned so far.Ā Thrombus formation is indeed much more complex than this.
So when multi-system organisms with complex body plans, like Mr. I.T.P., developed the necessity for hemostasis, which came first; the ability for blood vessels to constrict when injured, all the parts that are needed for adequate thrombus formation by platelets, or the complex clotting system which we are as yet to describe?Ā Be prepared to be totally amazed at what follows.Ā You’ll need a scorecard to keep track of the players involved.
Clotting Factors
While the thrombus is being formed, the clotting factors swing into action
to form a firmer fibrin clot around the soft thrombus.Ā Fibrin strands are insoluble
interlacing molecules that form from fibrinogen.Ā Yes, the same fibrinogen that
is needed to help the platelets form a thrombus in the first place.Ā Fibrinogen
is produced in the liver like all of the other clotting factors.Ā It stays in
solution until it is activated to become fibrin.Ā Don’t forget, the flow
of blood in the circulation is vital for life.Ā So, it’s important for
the body to know when to turn “on” the clotting mechanism for coagulation.Ā
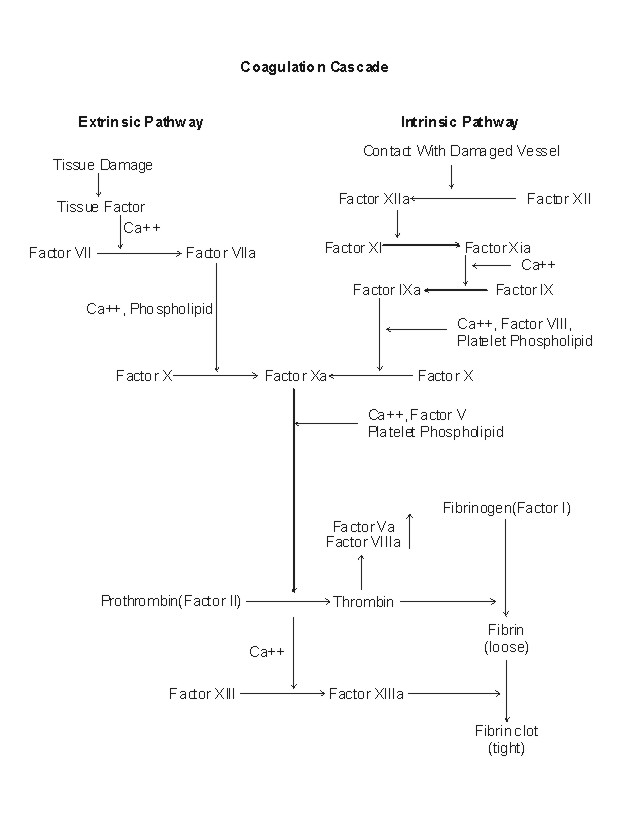
(for an overview of the coagulation cascade see Figure 1)

Figure 1. Note: the central role played by Factor X; how thrombin can potentiate itself by activating both factors V and VIII; and the overall interdependence of the clotting factors, calcium ions, and phospholipids, to make the whole system work.
What I want you to notice in Figure 1 is that there are many clotting factors within an intrinsic and extrinsic system, which when acted upon by either coming in contact with tissue damage, or the chemicals released from tissue damage, will result in the turning on of the coagulation cascade and clot formation.Ā In all, there appears to be at least 13 or more vital factors involved in the clotting mechanism of the body.ĀĀ Each and every one of them is needed for the body to properly accomplish controlled coagulation.Ā
As is readily apparent, fibrinogen, also known as (Clotting) Factor I, must be activated by a protein called thrombin in order to be converted into fibrin.Ā But thrombin itself is formed by the activation of prothrombin (Factor II) by Āactivated Factor X (Factor Xa) in combination with Factor V in the presence of platelet phospholipids.Ā
Now look again and you’ll notice that in order for Factor X to be activated it must be acted upon by either activated Factor VII or activated Factor IX with Factor VIII, (both in the presence of calcium ions and phospholipids).Ā But these factors in turn also need to be activated by other biomolecules and chemicals as well. (see Figure 1)
In considering the body’s ability to have blood clot at the right time and in the right set of circumstances we must take into account the liver’s capacity to produce enough of the clotting factors to provide adequate total body hemostasis.Ā The mechanisms that control liver production of clotting factors are poorly understood at this time.Ā But this too would play a major role in trying to figure out how this could have all developed over time.
There is ample medical evidence to show that with a significant decrease of any one of the clotting factors, the body would be at high risk of hemorrhage resulting in death.Ā Not a good way to win the battle for the survival of the fittest.Ā You may be familiar with two very common conditions that are due to clotting factor deficiencies; Hemophilia A and Hemophilia B, the former caused by deficiency of normal Factor VIII activity and the latter from deficiency of normal Factor IX activity.Ā Many of these people often have less than 1% of the normal clotting factor activity which has been noted to result in them suffering from frequent spontaneous hemorrhages in the joints and soft tissues and profuse hemorrhaging with trauma or surgery. ĀOften these people will die of spontaneous intracranial bleeding.Ā
In addition, besides these two relatively well-known hemophilias, there are also less common ones involving isolated deficiencies of Factors I, II, V, VII, X, XI, and XIII. Each of these conditions, that involve reductions in just one particular clotting factor activity, is known to put the patient at risk of death from minor trauma or spontaneous bleeding in a vital organ.Ā Treatment is available nowadays, but it wasn’t when multi-system organisms with complex body plans, the theoretical progenitors of modern man, were developing.Ā Macroevolutionists need to be able to explain how this system, involving numerous interdependent clotting factors, each of which is needed for proper coagulation, came into being one step at a time while still remaining functional, given the clinical evidence that seemingly would make this an impossibility. (revisit Figure 1)
A not uncommon condition that occurs in very sick patients is something called disseminated intravascular coagulation (DIC).Ā This is what the second patient described above died from.Ā The name of this condition and how itĀ manifests in clinical practice would seem to be a paradox since it involves widespread coagulation, but the patient bleeds to death.Ā It is a complex condition that is usually brought on by severe illness in which coagulation is enhanced throughout the body often resulting in organ damage. ĀBut this massive coagulation ultimately results in an overall drop in clotting factors, and often platelets as well, which cannot be compensated for quickly enough by the liver or the bone marrow respectively.Ā Although the platelet count will often drop, it is usually not to dangerous levels like we encountered in the case of Mr. I.T.P.Ā But the steep drop in most of the clotting factors by their consumption in this widespread coagulation syndrome often results in profound hemorrhaging which can often result in death.Ā
The presence and effects of the hemophilias and DIC on patient survival are modern medicine’s lesson to origin scientists about what can happen when the body does not have an adequate supply of various clotting factors.Ā Macroevolutionists certainly have their work cut out in order to theorize how the human coagulation cascade came into being one step at a time while still remaining functional for a multi-system organism.Ā The mere existence and the consequences of a person having any one of the hemophilias or developing the syndrome of DIC has shown that their proposed “one step at a time” mechanism of development would seem to be impossible given our understanding of how life really works.Ā Now add to this the absolute necessity of vascular constriction and adequate platelet function for proper hemostasis and you now have an irreducibly complex system that seemingly stands in defiance of macroevolution.ĀĀ
Anti-clotting Mechanisms
Don’t forget that just as it’s important to be able to stop bleeding
in the body, it’s also important to be able to keep the blood vessels clear
for blood flow.Ā Once the “on” switch for coagulation has been pushed,
how does it turn itself “off”?Ā Without these “on” or “off”
switches we’d always be running the risk of either bleeding to death, or
clotting off all of our blood vessels at once and causing death that way instead.Ā
In the right set of circumstances, clots can sometimes propagate along a vessel,
or break off and flow downstream thereby causing blockage of a blood vessel
which may result in permanent organ damage and even death.Ā
One of the ways that clotting may be slowed could be by the reduction of the clotting factors as they get used up in coagulation, in a similar fashion to the DIC syndrome mentioned above, but in a more controlled way.Ā However, this would be leaving too much to chance, since in order to reduce effective clotting you may end up bleeding to death instead.Ā And you would still need to contend with the liver’s ability to supply the circulation with more clotting factors.Ā No, the body has several natural anticoagulants which are able to inhibit coagulation in a way that allows for controlled clotting that generally does not result in the widespread blockage of blood vessels.Ā
One of these molecules is called AntiThrombin III, which with the help of another molecule, called heparin, is able to block the actions of both thrombin and activated Factor X.Ā Remember that thrombin is the molecule that converts fibrinogen to fibrin on the way to forming a clot, and activated Factor X is instrumental in convertingĀ prothrombin to thrombin.Ā So you can see that by blocking both of these procoagulant molecules, AntiThrombin III really does slow down clot formation. (revisit Figure 1)
Another mechanism that the body uses to slow down coagulation involves two molecules called; Protein C and Protein S.Ā Protein C binds to the protein C receptor on the endothelial cell membrane (lining cell of the blood vessel) and activates it.Ā Then in cooperation with nearby Protein S and in the presence of calcium ions, it neutralizes the clotting effects of activated Factor V and activated Factor VIII, both of which are important for coagulation. (revisit Figure 1)
So far we’ve looked at what happens when platelet function is compromised and when some or all of the clotting factors are defective or absent; hemorrhage leading to death.Ā What do you suppose would happen if there were a dysfunction of AntiThrombin III activity, or Protein C and Protein S function?Ā Look back and see what happened to Mrs. A.P.C-R.. ĀThe letters in her name stand for Activated C Protein Resistance.Ā
There are disorders in the body known as hypercoagulable states in which people tend to develop clots, usually in the veins of the legs, which can then break off and travel to the lungs causing sudden death by blocking the pulmonary arteries.Ā When this happens, even though the lungs may be bringing in oxygen to the alveoli, its ability to enter the bloodstream is severely limited because the blood that it’s supposed to go to has been blocked off by pulmonary emboli.Ā In this setting the oxygen needs of the body suddenly become compromised, the patient often becomes extremely short of breath, and death frequently follows very soon afterward.Ā The case study of Mrs. A.P.C-R. demonstrates how devastating this condition can be.Ā Ā
Conditions such as AntiThrombin III deficiency, Protein C deficiency, Protein S deficiency and Activated C Protein Resistance, all result in a hypercoaguable state because the natural anti-coagulation processes of the body are compromised and the pendulum swings toward coagulation in the body.Ā So now we have one more large group, consisting of these four factors of natural anti-coagulation (AntiThrombin III, heparin, Protein C and Protein S), to consider besides vasoconstriction, platelet function and the coagulation cascade, when trying to explain how hemostasis developed one step at a time.
Final Remarks
It is evident that the presence of all four of these components for properly
controlled hemostasis in the body, (vasoconstriction, platelet aggregation,
clotting factor activation, and anti-clotting mechanisms), demonstrates irreducible
complexity.Ā And also, within each one of these components exists an irreducibly
complex system of proteins, receptors and other chemicals that are all absolutely
necessary for each of these components to function adequately.Ā The entire system
demonstrates specified complexity in that all of the chemical components within
each system together perform a recognizable function that is vital for survival.Ā
And finally, the ability of the various components, by way of production capability,
receptor sensitivity, and reaction speed, each of which is important for survival,
points to the complexity of survival capacity contained within the hemostatic
system. ĀMacroevolution must be able to explain the step by step development
of this extremely complex and sensitive system while still allowing for function
and survival.Ā The presence of similar systems in similar or even divergent
organisms, although interesting to note, does not even begin to explain how
they came into being, and just as importantly, how they were able to function
adequately to allow for survival.
Next month we’ll look at how the body defends itself in: Sports are Simply a Reflection of Life (Without a good defense, you’re dead; literally!)
Dr. G.
Howard Glicksman M. D. graduated from the University of Toronto in 1978. He practiced primary care medicine for almost 25 yrs in Oakville, Ontario and Spring Hill, Florida. He recently left his private practice and has started to practice palliative medicine for a Hospice organization in his community. He has a special interest in how the ethos of our culture has been influenced by modern science’s understanding and promotion of what it means to be a human being.
Copyright 2004 Dr. Howard Glicksman. All rights reserved. International
copyright secured.
File Date: 5.01.04